Pain and Neuroplasticity
Neuroplasticity describes the constant molding and shaping taking place in the brain and central nervous system. Every day, our body’s form and break down trillions of tiny connections between nerves and brain cells. This continual flux is responsible for learning and memory, both consciously and unconsciously.
In the past, scientists believed that after a certain age, the central nervous system was largely fixed and stagnant. For example, nerve injuries could result in lifetime impairments. Victims of spinal cord injuries may lose the ability to stand or walk. People who had a strokes develop permanent areas of weakness.
But, this paradigm has already begun to shift. Neuroplasticity is a fundamental component of brain, spine and nerve function. Researchers are looking to harness the body’s ability to remodel itself, and we are starting to appreciate the power of this process. For example, stem cell technology combined with neurostimulation can restore the ability to walk in laboratory rats that were previously paralyzed from a spinal cord injury.
Patient case report
I had a patient, named Lucy[1], who demonstrated the mystery of neuroplasticity. She was a very pleasant lady, who ran a daycare for children, but had to retire when her struggle with severe spinal stenosis became too much. Despite undergoing a lumbar fusion surgery, she still reported back pain that spread down her legs. She came to our care after surgery and we tried physical therapy and rehab, alternative therapies (acupuncture, massage), medication therapy and injection therapy. In the end, we decided to trial and then implant a spinal cord stimulator.
Spinal Cord Stimulator
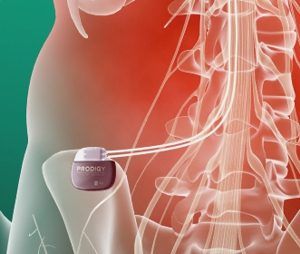
A spinal cord stimulator is a medical device used to treat chronic neuropathic pain conditions after other traditional efforts have failed. A trained specialist is able to place electrical leads in the epidural space connected to a small battery. The device sends electrical signals over the spinal cord and this works to neutralize pain signals and promote the body’s own mechanisms for blocking pain. Patients first undergo a 1 week trial, the leads are removed and then leads are permanently implanted and connected to the battery that is buried under the skin through a very small incision.
The results can be astonishing. When we first met Lucy, she was using a walker and considering a life confined to a wheelchair because her back and legs hurt too much when she walked. After implanting the spinal cord stimulator, her pain level decreased from a 7 out of 10 to a 4 out of 10. She was then able to follow up with her rehab care and within one month she began walking several blocks every evening. When I saw her six months later, she told me she was now working part-time at her old daycare.
Nerves in flux
Four years later, she returned to the clinic and reported that she did not feel as if the spinal cord stimulator was working as well as it had in the past. The device is programmed to direct electrical signals onto a focused area of the spinal cord, which in turn stimulates different regions of the body. In Lucy’s case, she used to feel a pleasant tingling sensation directly over the areas of the leg or back that hurt, but recently this went away.
Unfortunately we see this from time to time. Despite getting relief for years, over time, the benefit may go away. Most patients, like Lucy are grateful for the significant relief they had while it lasted, but in the end it is still frustrating.
We decided to try and salvage her therapy. There was nothing wrong with the system and the leads were in the same place from the original implant. We hypothesized that the pain processing neural pathways in the spinal cord “got used to” the stimulator program and new pathways formed in a different location. This was neuroplasticity in action.
Lucy came back to our outpatient surgery center and agreed to a revision. She lied on her belly in our operating room, was given light sedation and re-opened her small back incision. This gave us access to the leads and under X-ray fluoroscopy we pulled back on the leads, moving them down from one vertebra to the next. We let the anesthesia wear off and then turned on the stimulator. Lucy still did not feel the tingling in her legs. So, we moved them back another vertebrae. We retested and still no coverage of her pain.
Finally, when we pulled the leads back one more time, tested and then to our excitement, we got it. Lucy was overcome with emotion. She felt the pain relief that she once had and restored her life.
Few would predict that the leads could stimulate the legs in such a low position in the spine. This case serves as a clear example of the profound remodeling that can occur along the pain pathways.
[1] Lucy is an alias to protect my patient’s privacy


Recent Comments